So far each of my career changes have been due to a change in life circumstances, this time was no different. I needed an out from the demands of shift work on ITU, it was not fitting in with the demands of family life.
A lot had happened personally whilst working on ITU. Kate and I got married and we had a little boy but the months leading up to our new born baby arriving were some of the hardest in our lives. Pregnancy, delivery and post natal times were all tough. It was all worth it for the boy who came into our lives. So it was time to find something that was more suitable for bringing up a family.
Every month the current vacancies in the Trust were circulated in a printed booklet. I saw an advert advertising a post to become a clinical risk advisor. To be honest, until I started the interview preparations I had no idea what being a clinical risk advisor entailed but it looked like an interesting challenge.
Four weeks later I had a successful interview and three months later, after seven years of working in intensive care, I found myself heading into risk management.
There is no way to explain this job without first setting out why the role needs to exists.
Health warning note, some of this is challenging to read but it should not shake your faith in the NHS.
Not everything goes to plan in healthcare, sometimes mistakes occur. Some of these errors occur with no one individual at fault and have no harm associated with them, others unfortunately do cause harm. Sometimes, very rarely, these errors cause significant harm.
To prevent incidents occurring there are all sorts of virtual and real barriers in place. These could be physical barriers and designs to ensure staff and patients are safe, others involve training and written guidance describing how to perform tasks and carry out specific care actions. There is a whole body of research on this and how incidents occur. Industries additional to healthcare such as aerospace and vehicular manufacture have identified cultural and methodology theories that help to understand what causes incidents to occur and how to prevent them.
In simple terms, the main aim is to create safety barriers that prevent harm and promote safety.
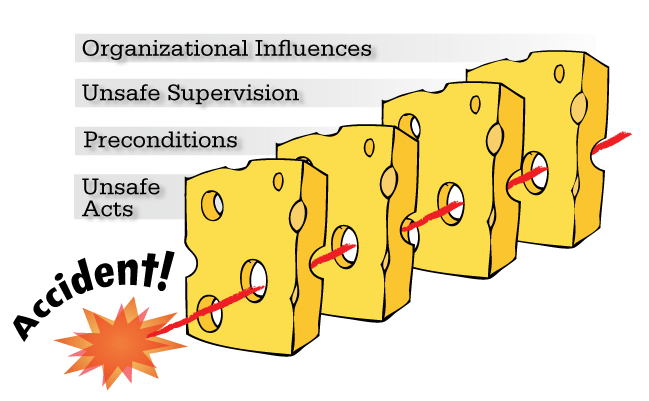
My role was to follow up incidents and work out how the barriers we had in place failed to prevent it happening.
Sometimes the solution to prevent an incident reoccurring required a safer piece of equipment, for example.
To give a patient drugs straight into their veins a small tube is inserted, this requires a needle to make a small hole in a patients arm. These needles were causing injuries in staff when they were not properly disposed of. Despite special bins in all the necessary place, training on how to use them and easy to follow advice, they still occurred. So I worked with the clinical leads in the Trust to changeover to a safer needle.
Other times, better understanding and training was needed.
My experience working in critical care allowed me to investigate and look deeper into incidents involving a delayed identification of patients deteriorating. This was not a theme unique to the Trust and many other hospitals were developing methods to prevent this type of incident. Within RBCH we introduced a new observation chart with scoring for each drop or rise in patients observations such as temperature, heart rate or blood pressure. This gave a tool for ward staff to score deterioration and use it to highlight if a patient was getting better or worse.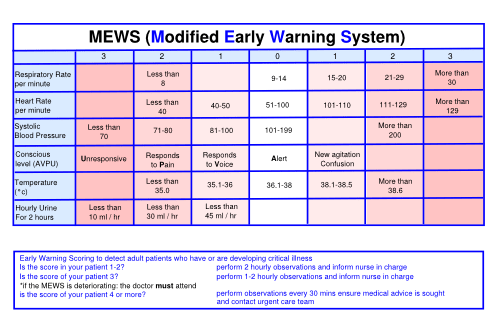
Sometimes, though incident investigation and response was far more complicated.
Those of you that have had an operation will probably have noticed that if this was one that required a right or a left sided operation, you would have had the site marked. A clear indication of where the surgeon needs to operate. Whilst a patient waits on the ward or is seen in clinic, the surgeon will also see the patient and read notes, thus again knowing where the operations needs to take place. In the theatre, covered in blue drapes with no face to see or notes to read very rarely a mistake occurs and the wrong site is operated on.
I followed up only one incident like this within the Trust. It required a great deal of difficult conversations with patients, relatives and the clinicians involved. But these occurred in other Trusts and so every effort was made to check and recheck procedures within the Trust to ensure this could not happen again.
This was most definitely a new direction. With different hours, and a job that no one else did in the Trust, in fact I struggled to find someone else in the country who did a similar role.
It took some time to get used to not being “clinical” and to see what I was doing as making a difference to patient care. Spending as much time as a I could on wards working with clinicians helped as well as talking to staff and patients about challenges they faced to get everything right.
It was a great job working with a great leader and team. I got to learn some very helpful work habits from my boss who helped me to develop my nursing skills into management skills. The post also opened me up to new experiences and I got to present the work I was doing on adverse incidents across the country. But after 2 years I felt I needed to get back to a more clinical based role.
My first internet search on NHS jobs came up with a result, the person specifications included ITU and management skills and it was closing that week! It was with the Health Protection Agency, I knew two people who had gone to work there so this felt like a path that fate was pushing me towards. It seemed like too much of a good opportunity to let go, so I applied.
A month later I was sitting an interview in front of 3 public health luminaries! One was involved in WHO work, another had led on local and national TB projects and another who had been involved with public and child health all across the south coast. Gulp!
You must be logged in to post a comment.